If you’ve ever wondered how doctors diagnose narcolepsy, you’re in the right place. Narcolepsy is a neurological disorder that affects the brain’s ability to regulate sleep-wake cycles, leading to excessive daytime sleepiness and uncontrollable sleep attacks. But how exactly do medical professionals determine if someone has narcolepsy? Let’s dive into the fascinating world of narcolepsy diagnosis.
When it comes to diagnosing narcolepsy, it’s not as simple as taking a quick nap and seeing if you fall asleep within minutes. No, there are several steps involved in the diagnostic process. First, your doctor will likely conduct a thorough medical history review to understand your symptoms and their duration. They may ask about your sleep patterns, any sudden muscle weakness or loss of muscle tone (known as cataplexy), and any other unusual experiences you may have had.
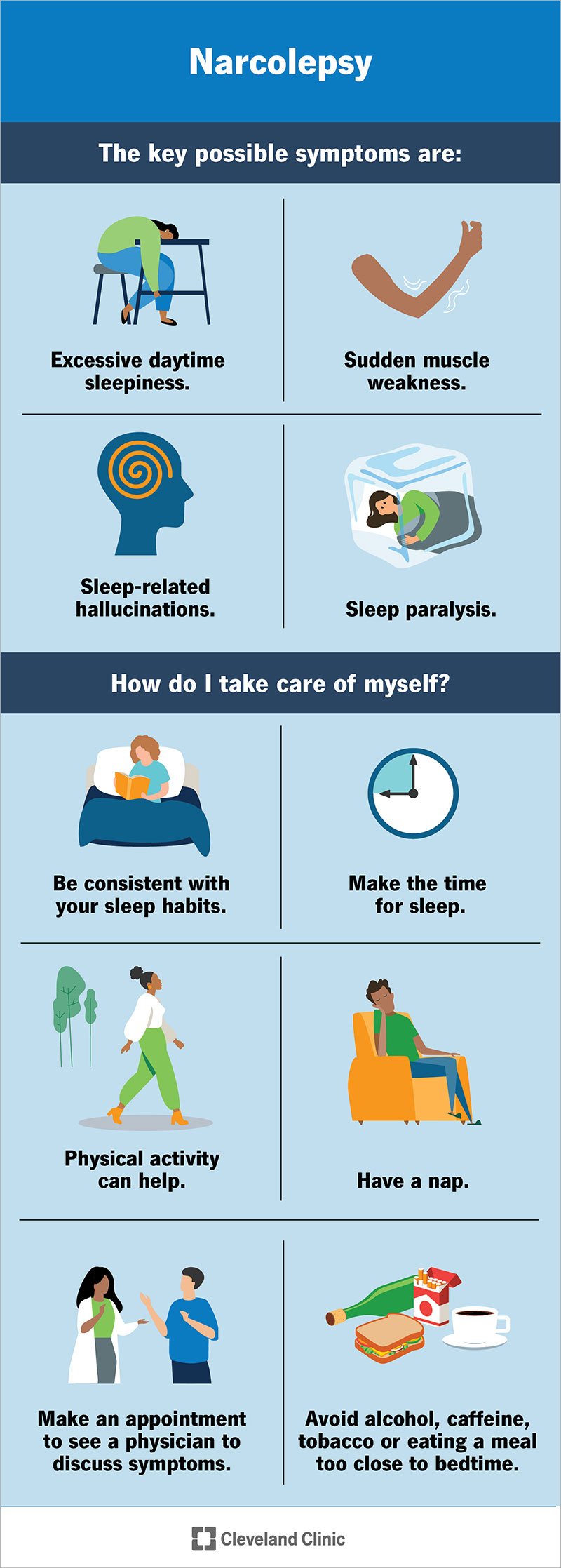
How is Narcolepsy Diagnosed?
Narcolepsy is a neurological disorder that affects the brain’s ability to regulate sleep-wake cycles. It is characterized by excessive daytime sleepiness, sudden episodes of sleep, and disrupted nighttime sleep. Diagnosing narcolepsy can be challenging, as its symptoms can be similar to other sleep disorders. However, with the help of a healthcare professional, a proper diagnosis can be made through a combination of medical history, physical examination, and specialized sleep tests.
When a person presents with symptoms suggestive of narcolepsy, the first step in the diagnostic process is a comprehensive medical history. The healthcare provider will ask about the frequency and duration of excessive daytime sleepiness, sudden sleep attacks, and other associated symptoms. They will also inquire about the presence of any family history of narcolepsy or other sleep disorders. This information helps in ruling out other potential causes of the symptoms and provides insights into the likelihood of narcolepsy.
Medical History and Physical Examination
During the medical history assessment, the healthcare provider may also ask about any medications the individual is taking and any underlying health conditions that may contribute to excessive sleepiness. Additionally, a physical examination may be conducted to check for any physical signs related to narcolepsy or other sleep disorders. The examination may include evaluating the individual’s sleep patterns, observing for sudden loss of muscle tone (cataplexy), and examining the throat and airways for any obstructions that may contribute to disrupted sleep.
Based on the information gathered from the medical history and physical examination, the healthcare provider may then refer the individual to a sleep specialist for further evaluation. A sleep specialist is a healthcare professional who specializes in diagnosing and treating sleep disorders.
Sleep Tests
One of the most important steps in diagnosing narcolepsy is the performance of sleep tests. Sleep tests are conducted in a sleep laboratory or a specialized sleep clinic and are designed to monitor and record various physiological parameters during sleep. The two main types of sleep tests used in the diagnosis of narcolepsy are the polysomnogram (PSG) and the multiple sleep latency test (MSLT).
A polysomnogram involves the use of electrodes and sensors placed on the individual’s body to monitor brain activity, eye movements, muscle tone, heart rate, and breathing patterns during sleep. This test helps in detecting any abnormalities in sleep architecture and can rule out other sleep disorders that may cause similar symptoms to narcolepsy.
The multiple sleep latency test is typically performed during the day following the overnight polysomnogram. It measures the individual’s tendency to fall asleep during quiet times and assesses the presence of rapid eye movement (REM) sleep during daytime naps. This test helps in confirming the diagnosis of narcolepsy by quantifying the severity of excessive daytime sleepiness and identifying the presence of REM sleep abnormalities.
Other Diagnostic Considerations
In some cases, additional diagnostic tests may be required to rule out other potential causes of excessive sleepiness. These tests may include blood tests to measure hormone levels, genetic testing to identify specific markers associated with narcolepsy, and imaging studies such as magnetic resonance imaging (MRI) to assess the brain’s structure and function.
It is important to note that the diagnosis of narcolepsy is not solely based on the results of these tests. The healthcare provider will consider the individual’s symptoms, medical history, and physical examination findings in conjunction with the sleep test results to make an accurate diagnosis.
In Summary
Diagnosing narcolepsy requires a comprehensive approach that involves a thorough medical history assessment, physical examination, and specialized sleep tests. The medical history helps in gathering information about the individual’s symptoms and ruling out other potential causes of excessive sleepiness. The physical examination may reveal physical signs related to narcolepsy or other sleep disorders. Sleep tests, such as the polysomnogram and the multiple sleep latency test, help in confirming the diagnosis by assessing sleep architecture and quantifying the severity of excessive daytime sleepiness. Additional diagnostic tests may be required to rule out other potential causes. Overall, a proper diagnosis of narcolepsy is essential for developing an appropriate treatment plan and managing the symptoms effectively.
Key Takeaways: How is narcolepsy diagnosed?
- Narcolepsy is diagnosed through a combination of sleep studies and medical history evaluations.
- Polysomnography is a sleep study that monitors brain activity, breathing, and movements during sleep.
- Multiple Sleep Latency Test (MSLT) measures how quickly a person falls asleep during the day.
- Achieving REM sleep quickly during the MSLT can be a sign of narcolepsy.
- Diagnosing narcolepsy may require consulting with a sleep specialist for a comprehensive evaluation.
Frequently Asked Questions
Here are some commonly asked questions about the diagnosis of narcolepsy:
What are the common methods used to diagnose narcolepsy?
Narcolepsy is typically diagnosed through a combination of medical history, physical examination, and sleep studies. The medical history will involve discussing the patient’s symptoms, sleep patterns, and any family history of narcolepsy. A physical examination may be conducted to rule out other potential causes of excessive daytime sleepiness. Sleep studies, such as a polysomnogram and multiple sleep latency test, are commonly used to measure brain activity, eye movements, and other physiological indicators to confirm the diagnosis of narcolepsy.
In addition, a blood test may be performed to check for certain genetic markers associated with narcolepsy, such as the HLA-DQB1*06:02 allele. This genetic test can help support the diagnosis, but it is not conclusive on its own.
Can narcolepsy be diagnosed in children?
Yes, narcolepsy can be diagnosed in children. However, it can be more challenging to recognize the symptoms in children compared to adults. Children may experience excessive daytime sleepiness, sudden loss of muscle tone (cataplexy), and other symptoms similar to adults with narcolepsy. The diagnosis process for children typically involves a thorough evaluation of their symptoms, sleep patterns, and medical history. Sleep studies may also be conducted to confirm the diagnosis.
It is important for parents to be aware of the possibility of narcolepsy in their children if they notice persistent excessive sleepiness or other unusual sleep-related symptoms. Consulting a pediatrician or sleep specialist can help in the diagnosis and management of narcolepsy in children.
Are there any specific criteria for diagnosing narcolepsy?
Yes, there are specific criteria for diagnosing narcolepsy. The International Classification of Sleep Disorders (ICSD) provides guidelines for the diagnosis of narcolepsy. According to the ICSD, the presence of excessive daytime sleepiness and either cataplexy or a positive result on a sleep study called a multiple sleep latency test (MSLT) is required for a diagnosis of narcolepsy. The MSLT measures the time it takes for a person to fall asleep in a quiet and comfortable environment during the day.
It is important for individuals suspected of having narcolepsy to undergo a comprehensive evaluation by a sleep specialist to ensure an accurate diagnosis based on the established criteria.
Can narcolepsy be misdiagnosed as another sleep disorder?
Yes, narcolepsy can sometimes be misdiagnosed as another sleep disorder due to overlapping symptoms. Conditions such as sleep apnea, idiopathic hypersomnia, and certain psychiatric disorders may present with excessive daytime sleepiness similar to narcolepsy. Additionally, other medical conditions and medication side effects can also cause excessive sleepiness.
To minimize the risk of misdiagnosis, a comprehensive evaluation is necessary, including a thorough medical history, physical examination, and sleep studies. The use of objective measures, such as polysomnography and the multiple sleep latency test, can help differentiate narcolepsy from other sleep disorders. Consulting with a sleep specialist experienced in diagnosing and treating narcolepsy is crucial for accurate diagnosis and appropriate management.
Is there a cure for narcolepsy?
Currently, there is no known cure for narcolepsy. However, the symptoms of narcolepsy can be effectively managed through a combination of lifestyle modifications, medication, and behavioral therapies. Medications such as stimulants and antidepressants can help reduce excessive daytime sleepiness and cataplexy. Lifestyle modifications, such as maintaining a regular sleep schedule, practicing good sleep hygiene, and avoiding sleep deprivation, can also help manage symptoms.
Behavioral therapies, such as scheduled napping and cognitive-behavioral therapy, may be recommended to improve sleep quality and cope with the challenges of narcolepsy. It is important for individuals with narcolepsy to work closely with their healthcare providers to develop an individualized treatment plan that addresses their specific symptoms and needs.
Final Summary: Understanding the Diagnosis of Narcolepsy
After diving into the world of narcolepsy diagnosis, it becomes clear that identifying this sleep disorder is no simple task. However, with the right knowledge and medical expertise, there are several key steps that can be taken to reach a diagnosis. From comprehensive medical history evaluations to overnight sleep studies, the diagnostic process involves a combination of tests and assessments to paint a complete picture.
One of the first steps in diagnosing narcolepsy is discussing your symptoms with a healthcare professional. This initial conversation helps them understand your experiences, such as excessive daytime sleepiness, sudden loss of muscle control, and vivid dream-like hallucinations. Following this, a comprehensive medical history evaluation is conducted to rule out other potential causes and identify any family history of narcolepsy.
Once the medical history is taken into account, a sleep study known as a polysomnogram may be recommended. This study involves spending a night in a sleep clinic while various sensors monitor brain waves, eye movements, and muscle activity. This data provides valuable insights into your sleep patterns and helps detect any abnormalities that may indicate narcolepsy. Additionally, a multiple sleep latency test (MSLT) may be conducted the following day to measure how quickly you fall asleep in a quiet environment. These tests, along with the evaluation of your symptoms, help healthcare professionals make an accurate diagnosis.
In conclusion, the road to diagnosing narcolepsy is a complex but necessary journey. By working closely with healthcare professionals, discussing symptoms, undergoing comprehensive evaluations, and participating in sleep studies, individuals can gain a clearer understanding of their condition. Remember, if you suspect you may have narcolepsy, don’t hesitate to seek medical advice. With the right diagnosis, proper treatment and management plans can be put into action, leading to improved quality of life and better control over the symptoms of this sleep disorder.



